In a small town in southwest Iowa, situated right on the Mississippi River, 60-year-old Shawn McVey has built a life for himself. After working for decades as a soil scientist with the U.S. Department of Agriculture, Shawn retired and moved closer to where he had grown up. His retirement has allowed him to pursue several hobbies. Shawn is a silversmith and lapidarist; he makes jewelry and polishes his own stones. He’s also a musician, starting a hand chime choir at his church and playing baritone horn in three different local bands. On December 14, 2025, people even came out to hear Christmas carols played solely on brass instruments, part of his town’s TUBACHRISTMAS.

Both his hobbies are painstakingly detail-oriented work. Shawn needs to read the right notes to keep pace with the band; with his jewelry, he needs to see whether the firescale has been fully worked out of the silver or the stones’ surfaces are polished to perfection. But what happens when thyroid eye disease (TED) throws a wrench in Shawn’s plans?
In the United States, an estimated 19 in every 100,000 people develop TED according to UCLA Health. But not every person experiences TED, or its recovery, in the same way. For Shawn, thyroid eye disease has sometimes necessitated him stepping back from his plans or the hobbies he loves to do. In other ways, his TED has become an inspiration to speak out and connect with others.
In his interview with Rareatives, Shawn discusses his diagnostic journey, the physical and mental implications of living with thyroid eye disease, the challenges of living with a rare disease in a rural area, and his hopes for the future.
Shawn’s Story
Have you ever heard of pseudomotor cerebri or an orbital inflammatory pseudotumor? Both terms refer to inflammatory conditions often called a “false tumor” because they mimic signs of a brain tumor, such as severe headaches, eye pain, and vision loss.
In 2023, while still living in Lincoln, Nebraska, Shawn developed a false tumor behind one eye that was pushing the eye out. He began seeing an eye specialist and, he explains, “We had pretty much resolved the situation. My eyelid had been stretched out, but I had eyelid surgery to address that.”
But, since his condition had improved so greatly, it was alarming for both Shawn and his specialist when both of his eyes began to swell. On top of that, Shawn’s eyes, dry and irritated, were painful and he was experiencing some double vision. Had his recovery not gone the way it was meant to? Was there something else at play?
Perhaps luckily, to point him in the right direction, Shawn was also seeing an endocrinologist at the time to manage his diabetes. One of the blood panels his endocrinologist had run included a thyroid measure, which came back out of range.
“She said it was probably nothing, but we needed to repeat the test,” Shawn tells me. Just to be sure, his endocrinologist also tested some additional thyroid measures. All of them came back out of range.
As Shawn considered what might be happening with his health, an idea kept nagging at him. His symptoms felt familiar in some way, although he couldn’t quite place it at first. Then, while he was speaking with his eye specialist, it suddenly struck him.
“I told him, ‘Maybe I have thyroid eye disease,’” Shawn says. “I’ve seen it on all these commercials.”
The diagnostic odyssey for someone with a rare condition, such as thyroid eye disease, spans 4-7 years on average. Some individuals receive diagnoses earlier than that, while others may wait for over a decade. Some doctors may not be aware of certain conditions. Rare and underserved conditions also mean less understanding of the potential diagnostic criteria. It is now becoming increasingly more common for individuals with rare diseases to research and find answers for themselves.
So, when Shawn asked whether TED was a possibility, his doctor took him seriously. And, as it turns out, Shawn was right — soon after, he was diagnosed with Graves’ disease and TED.
What is Thyroid Eye Disease?
Also known as Graves’ ophthalmopathy or Graves’ orbitopathy, thyroid eye disease is a rare autoimmune disease that affects the muscle and fat behind the eyes. Autoimmune conditions mean that the immune system mistakenly targets tissues or cells as “foreign invaders,” leading to damage and inflammation. If you have Graves’ disease, diabetes, or rheumatoid arthritis, you may be at a higher risk of developing TED.
In many cases, thyroid eye disease occurs in two phases: an inflammatory phase (lasting an estimated six months to two years), followed by a stable phase where inflammation may resolve. People with thyroid eye disease may experience symptoms such as:
- Puffy eyelids
- Sensitivity to light
- Eye pain and redness
- Bulging eyes
- Headaches
- Double vision
- Dry or watery eyes — “It’s hard to explain,” Shawn says, “when you have dry, irritated eyes that also won’t stop watering. How can they be both at the same time?”
- Feeling of “grittiness” in the eyes
- Eye misalignment
- Corneal damage/erosion (in severe cases)
The symptoms can be challenging to navigate, both physically and emotionally. Says Shawn, “It was very defeating. I had to do everything with one eye: shave, drive, read. It was hard to see outside in bright light. Many people with thyroid eye disease struggle with anxiety or depression when they begin losing their independence.”
What kept him going during this time, when he faced difficulty seeing his sheet music or finishing his jewelry? “I could still go fishing,” Shawn explains with a smile. “It didn’t matter if I had double vision there.”
If you have Thyroid Eye Disease or another rare condition and are struggling with your mental health, please consider leveraging some of the many resources offered by Global Genes. If you are a care partner or loved one, Give An Hour offers free mental health support.
Managing Thyroid Eye Disease
Treating thyroid eye disease requires a multidisciplinary approach, with several potential interventions: lubricating eye drops, selenium supplementation, corticosteroids, or even debulking surgery.
In Shawn’s case, his endocrinologist first addressed his thyroid concerns through medication. Shawn was then put on a treatment protocol for TEPEZZA (teprotumumab). Developed by biotechnology company Amgen, TEPEZZA is the first FDA-approved infusion for thyroid eye disease. The therapy works by targeting the IGF-1 receptor to address inflammation at the source.
As with any medication, TEPEZZA may cause side effects. The most common ones reported in clinical studies included muscle spasms, nausea, hair loss, diarrhea, feeling unusually tired, and increased blood sugar levels. Some people also experienced hearing changes, changes in taste, headaches, dry skin, weight loss, or nail changes. Most of these side effects were described as mild to moderate, and people with diabetes or prediabetes may need closer monitoring of their blood sugar while receiving treatment.
Shawn underwent eight infusions over a period of five months, with fantastic results. His doctor did note that there might be a 15% chance of recurrence within the first year, when some people experience flares, according to the literature. “But he told me there’s a bigger chance I was in the 85% group who would have no more issues,” Shawn says.
With that, he happily returned to his daily life — relocating in 2024 from Lincoln to where he lives today. And for most of the year, Shawn enjoyed his renewed lease on life. He spent time with friends, played his music, kayaked, and made his jewelry.

It wasn’t until December 2024, and into January 2025, that Shawn realized he was having difficulty seeing again. He vividly recalls preparing to play horn with a new band — then realizing he couldn’t see the music in front of him. When, shortly after, he had his photo taken with another group, he realized his eye was turned inward. He remembers looking at the photo and thinking, “Oh boy, I might have TED again.”
But this time, he knew what to do. He began reaching out to his community (and to his doctors) for another round of TEPEZZA, which he finishes this month. Again, he’s seeing beneficial results. He shares, “I went from one eye turned inward badly to passing the ‘normal’ test if you looked at my eyes now. They look very straight and the bulging has decreased. The orbital area swelling has evened out. I still have a bit of double vision left, but I haven’t completed all the infusions yet.”
One of the big hurdles of grappling with treatment and management is that recurrence remains possible. Shawn questions how long someone might need to stay on treatment for (is this lifelong?) or whether there’s any way to mitigate the risk of flares over time — questions that remain unclear. For patients, the uncertainty can be difficult.
Shawn says, “Thyroid eye disease and Graves’ disease are autoimmune diseases, so there is no cure. I remember asking my doctors what to do to make sure my TED never came back. They kind of laughed and said, ‘Well, that’s the million dollar question.’ There are ways to manage the symptoms — I’m on a maintenance dose of a medication to keep my thyroid in check so my Graves’ doesn’t come back — but there is no cure. That’s not really something I understood right away, and I feel like nobody really talks about this with people with autoimmune diseases.”
Lacking an Effective Healthcare Infrastructure
Adding another layer of difficulty to treating and managing thyroid eye disease is geographical location and the national spread of resources. You see, Shawn lives in a more rural area which he describes as a “healthcare desert.” A 2023 article published in The European Journal of Public Health defines healthcare deserts, or medical deserts, as:
areas where population healthcare needs are unmet partially or totally due to lack of adequate access or improper quality of healthcare services caused by insufficient human resources in health or facilities, long waiting times, disproportionate high costs of services or other socio-cultural barriers.
According to additional research performed by GoodRx in 2025, a stunning 80% of U.S. counties lack adequate healthcare services. In rural areas especially, individuals may face more significant challenges in finding a local specialist. According to a comparative study completed by The National Organization for Rare Disorders, “People with rare diseases often face geographic barriers to care. In the case of many rare diseases, there are only a handful of specialists nationwide, or even worldwide, who have expertise in a given rare condition. As a result, patients often travel long distances to access their treating providers. NORD’s recent survey shows that 80% of respondents were being treated by at least one specialist.”
“I help my folks get to their medical appointments. We have to drive over an hour, sometimes over an hour and a half one way, to see a specialist,” says Shawn, noting that it takes at least 90 minutes to get his family to see a dermatologist. “I found this to be the case for TED, too. If someone is going to be dealing with my eyes, I want them to be experienced. Trying to find anybody who knows about TED and has treated more than one or two other patients has been tough.”
Shawn points to the fact that there’s a shortage of qualified ophthalmologists who want to work in rural areas, often because these areas are less populated and may be less profitable for the physicians.
“They want to work in populated areas. When I was in Lincoln, the nurses were much more experienced. But rural areas are hit hard,” he says. “And the issue for patients is that travel can be expensive. There’s a time and cost associated, and what if you need a driver? Telemedicine is nice, but there are some things you can’t achieve with telemedicine.”
Individuals with rare conditions who live in rural areas may also face significant insurance constraints, limiting options further. When Shawn wanted to receive his TEPEZZA infusion at the local hospital, insurance denied his request. “So now I need to get the infusions in my home,” he says. “This has its own challenges. Now I have to have the supplies shipped, taking into consideration safety, like if the meds are refrigerated properly.”
A Changing Approach to Thyroid Eye Disease
To Shawn, sharing his story is so important because it expands awareness of thyroid eye disease, which has multiple benefits. First, highlighting thyroid eye disease, its impacts, and its unknowns could stimulate more curiosity and research within the scientific community. Shawn, in particular, hopes that researchers begin looking into the possibility of using artificial intelligence (AI) as a potential drug development or biomarker tool. “Could we use AI to engineer a new therapy or understand who’s at risk of having a flare?” he asks. “Some people flare frequently, but others go a long time without a problem. It would be good to see why that happens.”
Shawn also questions whether there could ever be some sort of autoimmune vaccine or preventative measure to stave off flares. Looking at the field of rare disease research currently, this actually could be a possibility. According to a July 2025 article published in Cells, “A novel therapeutic approach, inverse vaccination, is being developed to combat autoimmune diseases and other inflammatory conditions. It aims to educate the immune system to recognize self-components as innocuous and stop reacting against them.” This type of progress could not only help in cases like Shawn’s concerning Thyroid Eye Disease and Graves’, but also with the over 100 autoimmune diseases affecting an estimated 5-10% of the world’s total population.
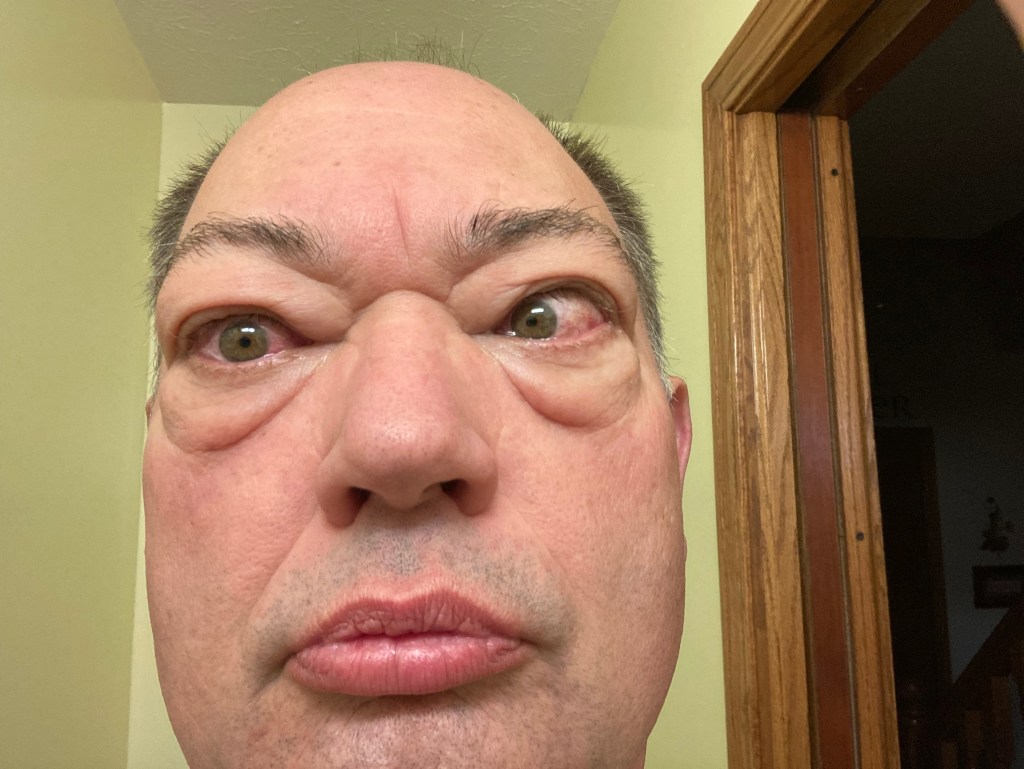
But, beyond scientific advancement, Shawn wanted to share his story because he doesn’t want other people to suffer or feel alone. When interviewed by a local TV station, he provided photos of himself in the midst of his thyroid eye disease, even though it was difficult. He points out his bulging eyes and says, “When I meet someone for the first time, maybe their frame of reference is that I’m just abnormal-looking. They don’t know what I used to look like. And that can be hard for people with TED — if we don’t look familiar to ourselves, how do we deal with that? So, for the interview, I wanted to give an example of what we’re talking about. Maybe it would help someone else recognize the key signs and symptoms. And if it helps someone, then it’s all OK.”
Shawn pauses, then he adds, “More awareness leads to earlier diagnosis. If you see the symptoms in yourself, or someone else, you can start pursuing treatment. Don’t wait. It’s not going to fix itself, and waiting can lead to permanent consequences. Be proactive. Is it going to be perfect when you’re done? Maybe not. But you’re going to be able to enjoy life.”

Shawn continues to be an advocate — to make an effort to speak up, to remain positive, and to spread understanding. He also stresses the importance of groups such as the TED Community Organization where “you have a sense of community, other people who have the same conditions, and you tend to learn from each other,” he says. Most of all, Shawn holds hope for the future.
“I’m not going to let TED beat me,” he says with a smile. “I’m still going to live.”
If you have been diagnosed with Thyroid Eye Disease, or would like to learn more about the condition, check out the TED Community Organization or thyroideyes.com.






Leave a comment