Every morning, before her 7-year-old daughter Alex eats a single bite of food, 29-year-old Faye Amado takes out a scale. She weighs out Alex’s meal to the gram, calculating the exact amount of protein Alex is permitted each day. But that’s not the end of Faye’s daily preparation. To keep Alex healthy, Faye must prepare a specialized medical formula and measure supplements.
“No one understands how to do this except me and her father,” says Faye. Right now, Faye’s husband is the home’s sole breadwinner. Faye stays home with Alex as a full-time caregiver since, she explains, “I cannot leave Alex, especially with anybody who cannot take good care of her.” Like many families in the rare disease space know, Alex’s care demands a level of knowledge and precision that cannot be delegated to just anybody.
The family, living in Iloilo City in the Philippines, has been learning to manage Alex’s rare genetic metabolic disease — known as maple syrup urine disease (MSUD) — for just over seven years now. Although the journey has been challenging, Faye has seen Alex reach some incredible milestones. But there’s still much to achieve, including the speech therapy Faye would like to enroll Alex in.

In her conversation with Rareatives, Faye discusses what maple syrup urine disease is, what she hopes Alex’s future will look like, and why she’s so proud of her young daughter.
Alex’s Story
On December 5, 2018, Faye and her husband welcomed their baby girl Alexandra Keila Barrido into the world. Alex was everything that Faye could have hoped for: a beautiful, bubbly child. Faye was so excited to introduce Alex to her older brother, Marky.

Doctors ran the necessary tests at the hospital — including a newborn screening panel, mandated by law in the Philippines in 2004 — and then sent the happy family home. For a few days, it seemed like Alex was a relatively healthy child. That’s because maple syrup urine disease typically does not appear with symptoms directly at birth. Instead, symptoms of the classic form appear over the next few days, usually once a newborn has begun consuming protein through breast milk or formula.
Faye, in fact, noticed some of these symptoms, though she didn’t consider them symptoms at the time. Alex was very sleepy and lethargic, sometimes having trouble opening her eyes. “She also didn’t want to breastfeed and had poor suck,” Faye explains. “I tried to switch to a formula using a bottle, which helped her drink, but still not a lot.”
Then, less than one week after the family went home, the hospital called Faye with an urgent request. As Faye shares, “The doctor told me the results of Alex’s newborn screening were urgent and Alex had maple syrup urine disease. Her leucine levels were dangerously high and she could die if not treated.”
An ambulance came to pick up Faye and Alex, taking them to the nearby Rural Health Center, where Alex was immediately admitted. What followed was one of the most frightening things a new parent could face. Doctors began taking blood and running tests. Although the physicians began telling Faye and her husband about maple syrup urine disease, they were still terrified of what the future might hold.
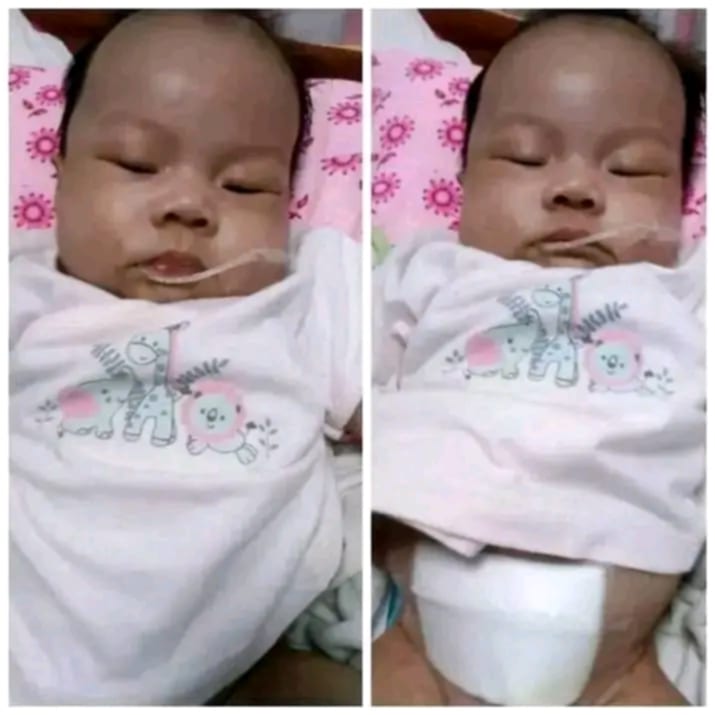
Since shortly after birth, Alex’s body had been accumulating toxic levels of branched-chain amino acids (specifically leucine). Normal leucine levels in the body range from 50 to 200 µmol/L. Alex’s levels were 3,000 µmol/L.
“The doctor explained to me that, when I gave her formula, her body had too much protein intake, leading to poor sucking and increased sleeping,” Faye says.
Although the damage from high leucine levels had already started, doctors decided, at just 9 days old, Alex needed to undergo peritoneal dialysis to flush toxins from the blood.
“We stayed at the pediatric ICU for more than three months,” says Faye. “But Alex was very strong. Even at nine days old. Even through everything, she kept fighting.”
What is Maple Syrup Urine Disease (MSUD)?
Maple syrup urine disease is a rare genetic metabolic disorder caused by either BCKDHA, BCKDHB, or DBT gene mutations. These gene mutations make the body unable to metabolize (break down) the amino acids leucine, isoleucine, and valine. The amino acids and toxic byproducts then accumulate in the system, leading to neurological dysfunction or metabolic crisis.
You might be wondering why the disease has such a sweet-sounding name. As it turns out, the build-up of amino acids can lead to a distinctive maple odor in the urine, sweat, or earwax. “I couldn’t figure out why they kept smelling Alex at the hospital,” Faye reflects.
Although MSUD is rare, affecting 1 in every 185,000 babies born worldwide, a study found that MSUD is the most common inborn error of metabolism in the Philippines, with 1 in every 55,241 babies born with this condition.
75% of people with MSUD have the classic neonatal form, where symptoms appear in early infancy. The remaining 25% of people have intermediate MSUD (appearing between ages five months and seven years), intermittent MSUD (appearing during metabolic stress), or thiamine-responsive MSUD. For those with the classic form, like Alex, early diagnosis and treatment is extremely important in stabilizing health and preventing long-term complications.
Infants with classic MSUD may present with symptoms and complications such as:
- Poor feeding
- Lethargy and irritability
- Muscle spasticity
- Hypertonia (increased muscle tone)
- Abnormal movements
- Developmental delays
- Osteoporosis
- Seizures
- Respiratory failures
Understanding Alex’s Health
As Faye and her husband began their rare disease path, there were several bumps in the road. In 2019, Alex spent one month in the hospital after pneumonia prompted a metabolic crisis. Faye learned quickly that any illness — even something as common as a cold — can be dangerous for children with MSUD.
For a child like Alex, who also has asthma, the risk of metabolic crisis remains high. Faye has had to take Alex to the emergency room several times over the years. This is why, recently, when Alex’s nebulizer broke, Faye was immediately concerned about keeping her daughter safe.
While Faye has gotten another nebulizer since, Rareatives would like to collaborate with others in the community to send her a backup nebulizer for Alex. If you have a nebulizer you would like to donate, please reach out to Rareatives to coordinate. Rareatives will happily cover the shipping costs to send Faye and Alex a backup nebulizer.
Treating and Managing MSUD
When leucine levels get extremely high, leucine can become neurotoxic, causing severe neurological damage. Without treatment, high leucine can lead to seizures, coma, or even death. Typically, the best time period for treatment is within the first few days of life to prevent irreversible neurological damage or death. But the earlier the better. After all, in the classic form, plasma leucine levels can begin rising within hours of birth — and encephalopathy, apnea, or other symptoms can set in within the first six days.
Faye says, “I hope by advocating and spreading awareness around maple syrup urine disease, I can teach people about MSUD and also remind doctors that newborn screening saves newborn babies’ lives. Newborn screening is the best way we can help babies get treated early.”
Managing MSUD requires a strict, protein-restricted diet, with some individuals needing to use specialized formulas — Alex gets nutritional support through ANAMIX JR (MSUD), though Faye says, “Her formula is not available in the Philippines. I have to order it abroad from the U.S. or U.K.” — to help control leucine levels. For individuals with hard-to-control leucine levels, hemodialysis (blood filtration treatments) may be used.
Alex must also undergo regular leucine monitoring through blood tests to ensure her leucine levels aren’t too high, since this could spark a metabolic crisis. She frequently visits her geneticist, dietitian, and developmental pediatrician. Navigating so many specialist needs can be difficult for rare disease families, as well as time-consuming and costly. Travel, visits, and medical needs cost money, sometimes that is hard to come by.
When Alex’s doctors want more detailed information — a full picture of all her amino acid levels — they request a plasma amino acids panel that Faye explains, “is too expensive, and we can’t afford it.” This highlights an important consideration. It is crucial to remember that not only are those in the rare disease community each fighting his or her own unique medical battle, but there are other factors they may face as well, such as costs, location and physical access to services, and specialist access and availability.
Liver transplantation can correct the metabolic defect, making it curative for MSUD — although even a liver transplant cannot fix existing neurological damage. However, getting a liver transplant can help some people with MSUD eat a normal diet and live without the risk of a metabolic crisis.
But liver transplantations are not universally accessible. Says Faye, “We don’t really have liver transplants in the Philippines.” Although The Medical Center can do liver transplants, only 68~ liver transplants were done between 1988 and 2023 in the Philippines, and the high cost often means people who need a liver transplant leave the country to receive one.
Faye prays that one day there will be a cure for MSUD. Until then, she says, “I’m hoping that scientists can come up with even a medicine to control the leucine levels, something to help patients process what they cannot now.”
Looking Towards the Future
Alex turned seven years old in December 2025. Even at her young age, she has been through more than what most people go through in a lifetime. And yet, she continues to fight. With pride, Faye says again, “She’s a very strong little girl.”

Alex lives with global development delay, with her cognitive development that of a child between one to two years old. For the first few years of her life, Alex could not walk on her own. The road forward was not easy. Alex was enrolled in intensive physical therapy sessions — sessions that Faye prioritized, channeling every family resource possible into getting Alex on her feet.
“All our funds went to her physical therapy and many hospital admissions,” Faye says. But when Alex started walking at age four, everything was worth it. Today, Faye says, “Alex can walk without any support.”

Faye’s next goal is to get Alex involved in speech therapy, to give her daughter a voice in the same way she helped give her the ability to walk, the way only a mother could: through sheer belief that it could be done.
“Speech therapy would be a big help for Alex to learn how to communicate. My dream is to wake up one day and hear her saying mama,” shares Faye. “I really want to help her, especially when she’s sick. I feel so bad that she can’t even tell me when she feels pain.” Faye is currently fundraising to help send Alex to speech therapy. Any donations are welcome.
Alex has taught Faye a lot about persistence and about love. Whenever times get tough, Faye looks at her daughter and is grateful that she is here. Faye also leans heavily on her faith, saying, “I want people to know that being a mother to a child with a rare condition is not easy. But God chose me to be Alex’s mother because He knows I will never give up on my daughter. Life is not easy, and our family is struggling, but I will never give up. I pray that no matter how hard it is, God will be with us and He will provide.”
And, importantly, Alex has also taught Faye about herself and her strength. “One thing I’ve learned through all this is that I can do it,” Faye says. “I’m a strong mama.”
If you or your child has been diagnosed with maple syrup urine disease, the MSUD Family Support Group offers resources and community for families navigating this condition.
To support Alex and her family directly, visit their fundraiser at gogetfunding.com/living-with-maple-syrup-urine-disease. You may also donate via PayPal using fayeamado7@gmail.com.





Leave a comment